Why You Might Have a Cavity Without Even Knowing It
Another cavity?!
Consider this article a public service announcement. I really dislike seeing patients lose teeth to tooth decay that could have been prevented.
My philosophy is simple: if a patient has a dental problem, I address it—but just as importantly, I give them the tools and knowledge to prevent future issues. Ideally, most visits after that are just for routine maintenance.
Why You Might Have a Cavity and Not Even Know It
Unfortunately, I often meet new patients with teeth so badly decayed there’s little chance of saving them. Just as frequently, I see people who finally schedule a checkup—often after years away from dental care—shocked to learn they have cavities. Many assume they lost a filling, when in fact, a chunk of enamel has broken off.
So why the surprise?
Most people believe cavities are supposed to hurt. Sometimes they do. But in the early stages, they’re usually painless. By the time a tooth actually hurts, the cavity has likely reached a serious stage. Often, I’m deciding whether to attempt a root canal—or whether extraction is the only option. A basic understanding of dental anatomy helps explain why.
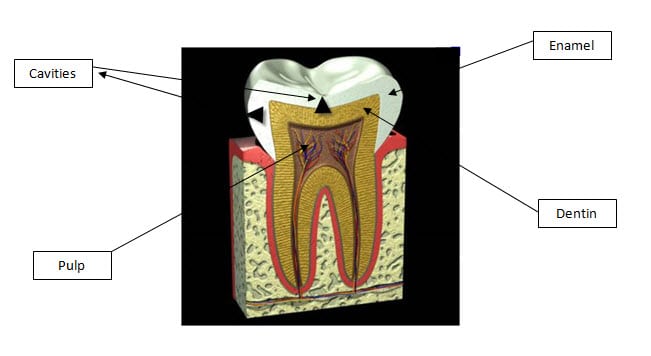
Scroll down to the illustration below.
The outer layer of your tooth—enamel—is the hardest substance in your body. It’s made to last a lifetime and helps you chew your food efficiently. But here’s the key: it doesn’t have nerves. Enamel is more than 95% mineral. The rest is water and organic material. Because it lacks nerves, it doesn’t feel anything. That’s useful—you wouldn’t want pain every time you bit into food. But it also means decay can silently destroy it without causing any warning signs.
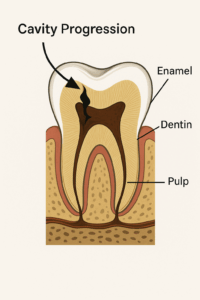
Even when decay reaches the underlying layer—dentin—you may still feel nothing. Only when it approaches the soft center—the pulp, where nerves and blood vessels live—do you usually feel pain. By then, the damage from a cavity is often extensive.
To make matters worse, decay doesn’t spread in a straight line. Take a look at the black triangles in the diagram. A cavity often starts at a small point on the outside and fans out wide inside the enamel. The tooth might look intact—until the undermined enamel collapses due to internal damage.
How Dentists Detect a Cavity Early
Cavities often form between teeth—places you can’t see. Even I need x-rays to catch them in those areas. Dentists rely on visual checks, dental probes, x-rays, and sometimes laser detection to find decay. Even then, spotting it under old fillings can be tricky.
Modern dental technology has made early cavity detection far easier. Digital x-rays produce high-resolution images with minimal radiation. Laser-based devices, such as DIAGNOdent, can detect tiny lesions before they become visible to the eye. These advances allow dentists to restore enamel with less invasive procedures—often saving the tooth before it ever hurts.
Preventing Future Cavities
Regular dental visits, daily brushing and flossing, and a balanced diet are the best ways to stop cavities before they start. Using fluoride toothpaste and limiting sugar intake help protect enamel. If you’d like to learn more about keeping your enamel strong naturally, read this related article.
Another simple habit that makes a difference is drinking water throughout the day. It rinses away food particles and helps neutralize acids that can erode enamel. If you sip coffee, soda, or juice often, consider rinsing with water afterward. Saliva production also matters—dry mouth, caused by medications or dehydration, increases your risk of cavities.
For people prone to recurrent decay, your dentist may recommend professional fluoride treatments or prescription-strength remineralizing pastes. These can rebuild weakened enamel and reduce sensitivity before a cavity takes hold.
The Takeaway
If someone you care about hasn’t seen a dentist in a while, ask them to read this article. You might help them avoid discomfort, costly procedures, and even tooth loss. Don’t wait for pain to signal that something’s wrong—a silent cavity can be far more damaging than one that hurts.
And for those thinking, “If it gets bad, I’ll just pull it,”—well, sometimes that’s necessary. But that’s a conversation for another day.
🦷 Learn more: How Cavities Form – American Dental Association