Can You Regrow Teeth? The Truth About USAG-1, Tooth Regrowth, and What’s in Clinical Trials
Can you regrow teeth? That’s the question behind the latest USAG-1 headlines—and the answer is more nuanced than Instagram makes it sound.
If you’ve been on Instagram or TikTok lately, you may have seen someone confidently claim: “Yes, you can regrow teeth — look up Toregem BioPharma and their USAG-1 blocker.”
That kind of statement mixes a real scientific idea with an unrealistic “it’s available now” conclusion. So let’s slow it down and separate what’s credible from what’s clickbait.
This article is a grounded follow-up to the recent wave of viral “tooth regrowth” content (including topical patches and miracle claims). Unlike those trends, the USAG-1 story is rooted in legitimate developmental biology — but it’s still early-stage.
Can you regrow teeth today?
Right now, the practical answer is: not in routine clinical dentistry.
However, researchers are actively investigating whether certain biological “brakes” on tooth development can be lifted to allow dormant tooth-forming pathways to restart. That’s what the USAG-1 research is about.
What is USAG-1, and why does it matter?
USAG-1 is a protein involved in signaling pathways that influence tooth development. Think of it as part of the body’s regulatory system that helps determine when tooth formation should stop.
Humans typically form two sets of teeth (primary and permanent). After that, the body doesn’t normally keep producing new tooth buds the way some animals do. Researchers have been trying to understand whether this “shutdown” is absolute — or whether certain pathways can be reactivated under controlled conditions.
In preclinical research (animal studies), blocking USAG-1 has been associated with additional tooth formation in some models. That doesn’t mean the same outcome is guaranteed in humans — but it’s why scientists consider USAG-1 a serious target for regenerative dentistry research.
If you want a reputable overview of regenerative dental research as a field, the National Institute of Dental and Craniofacial Research (NIDCR) is a good starting point:
NIDCR — National Institute of Dental and Craniofacial Research.
Meet TRG035: what people are actually talking about
TRG035 is commonly described in media coverage as an investigational therapy connected to the USAG-1 pathway. It’s discussed as a biologic approach (often framed as an antibody-based strategy) aimed at reducing USAG-1’s inhibitory effect so tooth-development signaling can proceed.
Important clarification: this is not a topical patch, not a toothpaste, not a supplement, and not something you can order online.
Are there human clinical trials?
Yes — but this is where social media often oversimplifies things.
Public reports describe human clinical trial work beginning in Japan, with early-stage human research focusing first on safety and feasibility, and with longer-term hopes of broader dental use later in the decade if trials go well. Here’s a mainstream dental-industry write-up:
Dentistry Today — Japanese researchers and a potential “third set of teeth” medicine.
In drug development terms:
- Phase 1 primarily evaluates safety, dosing, and side effects.
- Phase 2 begins to evaluate whether the treatment works reliably (efficacy), and in whom.
- Phase 3 compares outcomes in larger groups and supports regulatory approval decisions.
So, if you’re hearing “it’s available for limited use in the United States,” treat that as a red flag. “In trials” does not mean “available in clinics.” In the U.S., legitimate access usually happens through formal clinical trial enrollment, not routine prescription or dental office offerings.
If you’d like to check clinical trials directly, the best public database is:
ClinicalTrials.gov.
Can you regrow teeth in adults with this approach?
This is the key question — and the one we don’t have definitive answers for yet.
Even if a treatment can stimulate tooth formation in humans, dentistry still needs answers to the clinical questions that actually matter, like:
- Where would a new tooth form (and can that be controlled)?
- Would it develop a functional root and integrate properly with bone and ligament?
- How predictable would the results be in older adults vs. younger patients?
- What are the system-wide effects of changing a signaling pathway that may influence other tissues?
That’s why early trials are cautious and staged. Dentistry needs predictable placement, function, and long-term safety — not just a headline that says “teeth regrow.”
Can you regrow teeth naturally?
This is one of the most common searches after people see a viral video: can you regrow teeth naturally without surgery, implants, or dental treatment?
In everyday clinical reality, the answer is still no. Enamel does not biologically regrow once it’s lost, and a fully missing adult tooth does not spontaneously return. What you can do is reduce risk and slow damage (for example, improving hygiene, reducing acidic exposures, and addressing dry mouth and periodontal inflammation early).
Why viral “tooth regrowth” content spreads so fast
Tooth loss is personal. It affects confidence, chewing, nutrition, speech, and quality of life. So it’s understandable that people want a breakthrough that replaces implants, bridges, or dentures with something biologically natural.
That emotional hook is exactly why misinformation spreads quickly. A short video can imply that a therapy is already “out there,” when in reality the science is still in the careful, stepwise process of clinical validation.
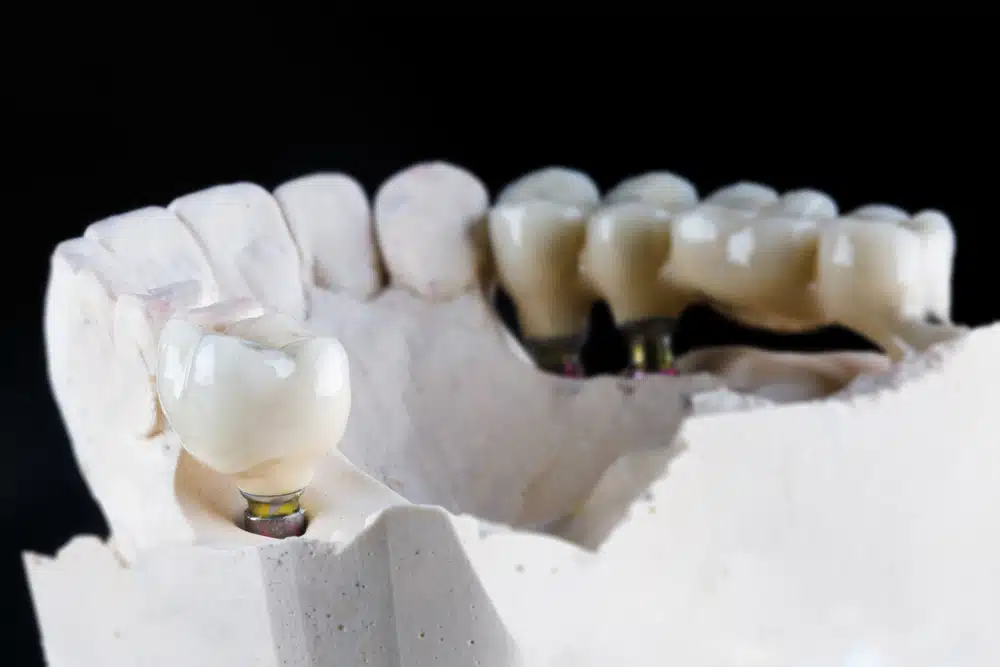
How this connects to today’s real-world options
While we wait for regenerative approaches to mature, modern dentistry already offers excellent solutions for missing teeth and structurally compromised teeth.
If you want a broader overview of tooth replacement and emerging innovation, here’s your 2024 article that covers regrowing teeth concepts alongside modern alternatives:
And if you’re looking at overall health support as part of a “keep your teeth longer” strategy (inflammation, micronutrients, and wellness basics), you can also explore your supplement resource hub here:
What you can do right now (while science catches up)
If you’re hoping to avoid tooth loss in the first place, the highest ROI remains boring — and effective:
- Consistent home care (brushing + interdental cleaning)
- Periodontal prevention and early intervention
- Managing dry mouth, acidity, and frequent snacking patterns
- Staying current on exams so small problems don’t become big ones
Regenerative dentistry may one day change the landscape. But until then, prevention and early diagnosis still beat any “future miracle.”
Quick FAQ: Can you regrow teeth?
Can you regrow teeth if you lost one as an adult?
Today, no — not as a predictable, widely available clinical treatment. Research is exploring biological regeneration approaches, but they are still in early human trial stages.
Can you regrow teeth with a patch, serum, or supplement?
Be skeptical. Viral products often imply “regrowth,” but typically lack clinical evidence. A true regenerative treatment would require rigorous trials, safety review, and predictable outcomes—not just marketing claims.
Can you regrow teeth in the United States right now?
In routine practice, no. If future access happens, it would be through regulated pathways, typically beginning with formal clinical trials.
Bottom line
Can you regrow teeth? Not as a standard dental service today.
But the USAG-1 research is one of the more credible scientific directions being discussed publicly, and it’s being explored through structured clinical research rather than consumer products and viral hacks.
So, can you regrow teeth today? Not as a routine dental treatment—but the clinical-trial pathway is real, and it’s worth watching carefully.
Educational note: This article is for general information and is not medical or dental advice. If you have tooth pain, swelling, infection, or tooth mobility, you should be evaluated by a licensed dental professional.