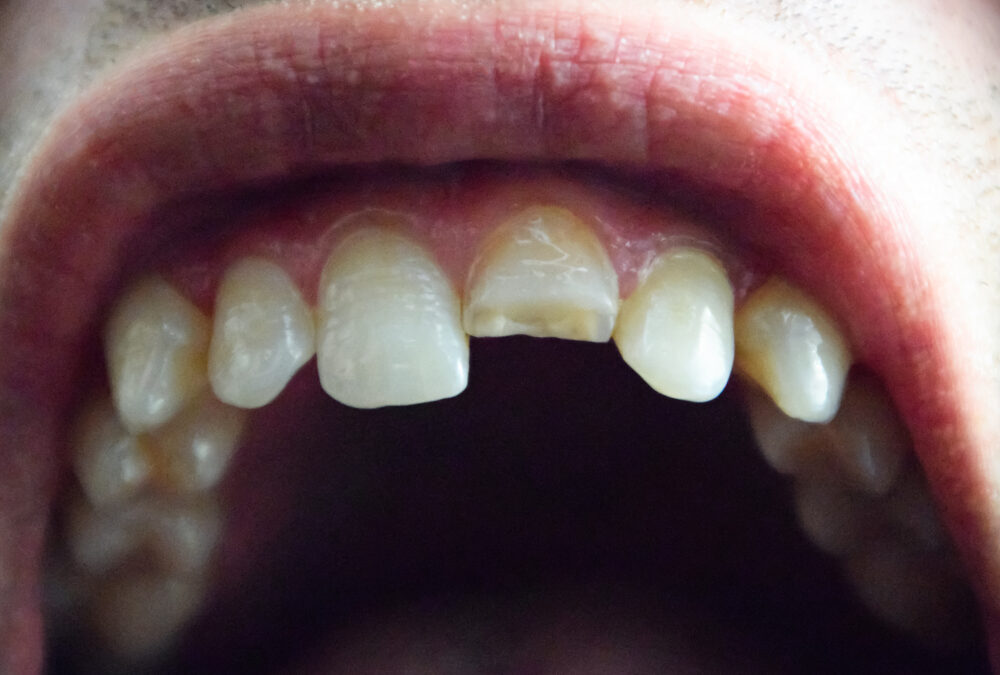
The treatment of cracked teeth can be one of the most complex — and frustrating — experiences for any patient, or dentist, for that matter. Symptoms can be erratic, elusive and the solutions can range from simple to very involved. It is not uncommon for patients with cracked teeth to visit several dentists stating symptoms that can’t be reproduced or even seen by the dentist.
If you suspect you may have a cracked tooth, read this carefully. It pays to be fully informed and prepared for any and all possibilities.
Q: My teeth aren’t cracked. Why should I care?
A: Cracked teeth are becoming a growing problem in the adult population. What used to be encountered by most dentists only occasionally is now a common occurrence in almost every dental office. Just a few short years ago dental journals were reporting near “epidemic” findings of as many as one-in-four patients that grind their teeth. (One of the principal causes of cracked teeth.) Today, those estimates approach one in three. If it doesn’t affect you now, it just might down the road.
Q: Why do teeth get cracks?
A: Traditionally, one of the most common causes of cracked teeth had to do with teeth that were heavily filled. Decay and subsequent filling cause a weakening of remaining tooth structure. Any new decay that a patient develops after a tooth has been filled can weaken it still further. Since teeth — filled or not — are used for chewing, they are subject to physical stress. All materials subject to stress can suffer from stress fatigue. After many bites on the tooth and filling (stress cycles), a hairline fracture can develop. And that’s just the “normal” stress. If a person is under mental stress, they may grind or clench their teeth (usually when sleeping). This can, and does, result in even higher levels of tooth stress.
Q: Why does the tooth sometimes hurt to hot and/or cold?
A: The nerve of the tooth becomes aggravated by the crack and by the bacteria being forced into it through tubules of dentin. The nerve then gets inflamed because of the toxins in the bacteria. A classic symptom of nerve inflammation is hot and cold sensitivity.
Q: Why does it hurt to bite on my tooth?
A: As your tooth flexes (yes it does bend to a very slight degree!) your nerve becomes stimulated by fluid that backs up in the tubules of dentin. Dentin is the inner layer of tooth structure, below your enamel. The tubules run down to the nerve and the fluid moves in them. You perceive that as a sharp pain.
Q: What will happen if I just ignore it?
A: Typically, the crack continues to progress slowly until, like a crack in a car windshield, it spreads throughout the glass or, in this case, the tooth. Sometimes, the crack travels sideways and a piece of the tooth breaks off. At other times, it runs deep into the root — possibly reaching the nerve itself. Teeth can often go for months in a stable, but inflamed condition. Sometimes they seem to get better, only to suddenly get worse. It is hard to predict the course of an untreated tooth, but it is usually a slow degeneration as the crack gets deeper. If caught early enough, a small crack will usually respond well to treatment, but a bigger one can lead to root canal treatment or even extraction. The nerve can be attacked by the bacteria, which tends to make the tooth very sensitive to hot and/or cold. The ache can be persistent as the tooth dies and the pain can range from moderate to severe. Subsequent infections can spread into the underlying bone causing an abscess. In this case, the pain is usually severe, and is not effectively controlled by pain killers.
Q: What is the best way to treat a cracked tooth?
A: Unless the crack is stabilized and splinted together, the tooth is likely to deteriorate. Although various methods may be attempted to bond the crack together, this is only likely to work if the crack is very superficial. Chewing forces are quite strong, though, and if the tooth has been sensitive these “patch-up” efforts tend to be unpredictable and may not work at all. The only real solution is to bind the entire tooth together with a crown so that any chewing force is transferred to the entire tooth, rather than acting to split it apart.
Q: What color will the crown be?
A: Most people seem to prefer that their teeth have a natural appearance. We can manufacture one of several types of crowns — many of which are metal-free — and which are extremely strong. Because many cracked teeth have large black mercury-amalgam fillings, your tooth is likely to look much better after being crowned. At least there is some small benefit to the time and expense involved.
Q: Are there any other advantages to having a full crown?
A: The crown is bonded over the entire tooth. This seals the cracks and the various sources of bacterial leakage that can result from the patchwork of fillings typically found in these teeth. The nerve is now provided with its best chance of recovery since there is a hermetic (airtight) seal, and the crack has been immobilized. Still, it is not necessarily completely immobilized. You still use it to eat . . . .
Q: Is there any guarantee that the nerve will recover?
A: No! Despite the best treatment and efforts, at least 10% of cracked teeth have nerves that will die. The tooth can (and does) still move slightly within the bone, and this slight movement can flex the crack from the opposite site — despite a crown on top.
Sometimes, the existing bacterial damage is already sufficiently advanced, and the damage to the nerve so severe that the nerve goes on to die regardless of what is done. This is the main reason why early treatment is recommended to minimize the size of the crack and bacterial invasion.
Q: What happens if the nerve doesn’t recover?
A: Generally, the nerve will die and you run the risk of developing an abscess. The traditional therapy is a root canal (also called endodontic therapy). Usually, a small hole is made in the crown in order to treat it. The hole is later filled with a permanent tooth-colored filling.
Q: Will this weaken my crown?
A: Possibly, a little. But it is a quick and uncomplicated way to handle the problem, with few long-term problems. The white filling usually matches the crown well, but don’t expect it to be invisible. For most people, it’s not a problem, but if having a filling in your crown bothers you, a new crown can be made if you don’t mind the additional expense.
A second option is to cement the crown with a temporary cement. If the nerve dies, the crown can be removed for the root canal treatment. This prevents a need for drilling through the crown, but has other down-sides. You have to decide if you are prepared to accept them: First, if the crown is put on with a temporary cement, it will come off one day. Depending upon the type of cement and inherent retention of the crown, this could range from months to years. In most cases, if the crown loosens, you will notice it, retrieve it, and all is well. However, it is possible to bite on it, break it, or accidentally swallow it — so you need to take this into account before making your decision, because you may be have to face the cost of a repair or a new crown.
Q: What if the crown loosens after it has been temporarily cemented and nothing else bad happens?
A: Well, then, you can choose to re-cement it temporarily or with a final cement. If enough time has elapsed so you are pretty certain your symptoms are gone and the nerve is doing well, you may elect to use the stronger cement. Talk this over with your dentist, because that zone of evaluation can range from three months to three years. Sometimes it is simply a matter of clinical judgment. Every case is different and complex individual case factors need to be taken into account. Even with the best efforts some nerves will go on to die (even as long as ten or more years later). You should also note that most dentists include the cost of cementing your crown only once. If you elect to cement it with temporary cement, an extra expense will be involved (either re-cementation, office visit, or both — depending upon your doctor’s policy) unless your dentist has told you otherwise.
Q: How successful is endodontic (root canal) therapy?
A: Pretty successful. Though 5 to 15% can still fail (even without a crack) according to various studies. Having a crack pushes this number toward the higher end. Some of these root canaled teeth – especially those with a history of a prior crack – will continue to get pain when bitten on or, sometimes when pushed from the side. This is due to the crack movement irritating the tissues around the tooth (the periodontal ligament). At this point, there is no treatment other than extraction for these cases.
Q: So I can go through all that time, discomfort, expense, and still lose the tooth?
A: Yes.
Q: What then?
A: There are several options for replacement.
-
- An implant placed into the bone, which supports a new tooth.
-
- A conventional bridge (which caps teeth on either side of the missing tooth).
Many of the advantages and disadvantages of these options are discussed elsewhere on this site.
Please remember, information provided on the internet is not a substitute for clinical evaluation by a licensed professional.
Your situation is unique to you and deserves proper attention and treatment.